Published July 10, 2025
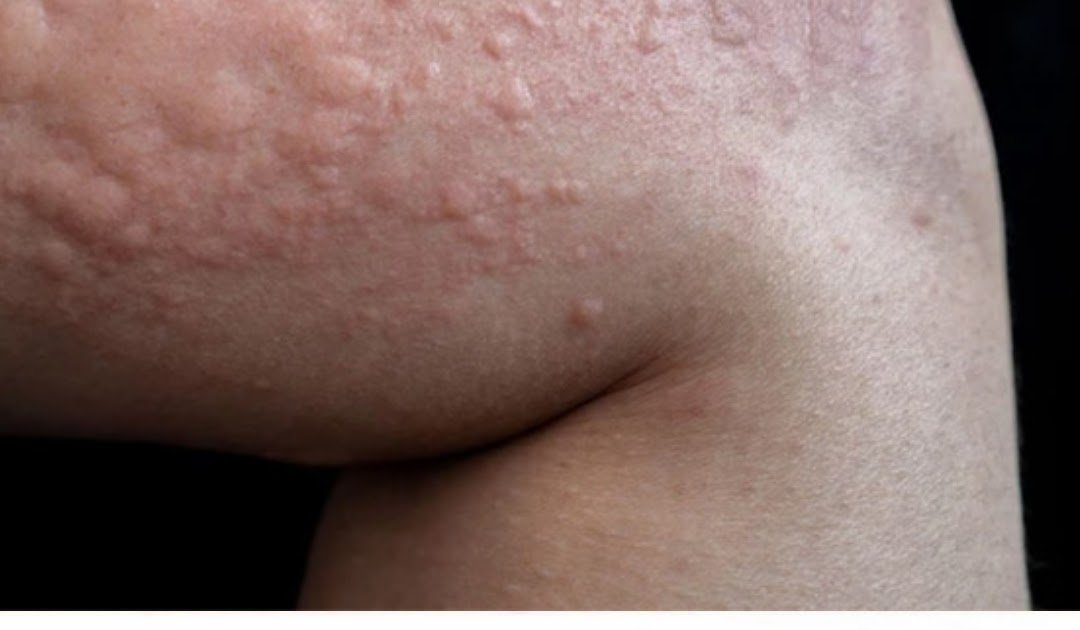
Waking up with red, itchy patches on your skin is a familiar scene for anyone who has experienced hives. One moment your skin looks normal, the next it’s covered in raised, swollen welts that burn, sting, and seem to move around the body.
Hives (urticaria) may look harmless, but they are a clear sign that your body has activated an internal alarm. Mast cells in the skin release histamine, blood vessels dilate, fluid leaks into surrounding tissue, and that uncomfortable “on fire” sensation appears.
Most episodes disappear within hours or days. Others persist for weeks, turning into a frustrating puzzle with no obvious cause. Understanding what triggers hives, how to calm the reaction, and when to seek help can make all the difference.
Acute vs. Chronic Hives: Where Things Change
Acute hives last less than six weeks and usually have a clear trigger:
-
Food reactions
-
Medications
-
Sudden temperature changes
-
Infections
Chronic hives last longer than six weeks and often return in cycles. In nearly half of cases, no clear cause is found. This is where autoimmune mechanisms may be involved. The immune system mistakenly attacks the body’s own cells, keeping mast cells in a constant state of alert.
What’s Really Happening Under the Skin?
The process behind hives is surprisingly consistent:
-
A substance or stimulus irritates the body
-
Mast cells release histamine into the skin
-
Blood vessels expand and leak fluid
-
Red, swollen welts form
-
Intense itching appears as histamine stimulates nerve endings
This is why hives can look dramatic but vanish just as quickly as they appear.
Surprising Triggers Most People Overlook
Many people assume hives only come from allergies. In reality, the list of triggers is much wider.
1. Foods
-
Shellfish
-
Nuts
-
Eggs
-
Milk
-
Artificial dyes and preservatives
Even foods you’ve tolerated for years can suddenly cause reactions.
2. Medications
-
Non-steroidal anti-inflammatory drugs (NSAIDs)
-
Antibiotics
-
Radiologic contrast agents
Sometimes the reaction appears hours after taking the drug, making the link easy to miss.
3. Infections
-
Common colds
-
Sinus infections
-
Viral gastroenteritis
Your immune system’s response to infection can trigger histamine release.
4. Stress
Stress doesn’t create hives out of thin air, but it strongly amplifies histamine release. Emotional tension makes mast cells more reactive, increasing both frequency and intensity of outbreaks.
5. Physical Factors
-
Heat and sweating
-
Cold air or water
-
Pressure from tight clothing or backpack straps
-
Friction
-
Intense sunlight
Some people develop hives simply from sitting on a hard surface or carrying a heavy bag.
6. Dermatographism
In this condition, light scratching causes raised, red lines within minutes. It’s one of the most common but least recognized forms of hives.
How to Calm a Flare-Up and Prevent New Ones
Before rushing to the doctor, there are practical steps you can take at home. These do not replace medical care if hives persist.
First-Line Antihistamines
Modern antihistamines such as loratadine, cetirizine, or fexofenadine usually reduce itching and swelling within hours. They are non-drowsy and safer for daily activities.
Avoid older sedating antihistamines if you need to work or drive.
Keep a Trigger Journal
Write down:
-
What you ate
-
Weather conditions
-
Medications taken
-
Stressful situations
Patterns often appear after a few episodes, making it easier to eliminate triggers.
Skin Care Matters
-
Apply cold compresses to reduce burning
-
Take lukewarm baths with colloidal oatmeal
-
Use fragrance-free moisturizers
-
Avoid hot showers and harsh soaps
Simple care can significantly reduce irritation.
When Should You See a Doctor?
Seek medical evaluation if:
-
Hives last more than six weeks
-
They return every week or frequently
-
Swelling affects lips, eyelids, or tongue (possible angioedema)
-
You have shortness of breath, wheezing, or abdominal pain
These may indicate a systemic reaction requiring urgent attention.
FAQ – Common Questions About Hives
Can hives mean a serious allergy?
Most cases are limited to the skin. However, if hives occur with throat swelling or breathing difficulty, seek emergency care. This can progress to anaphylaxis.
Can I use steroid creams?
Topical steroids usually help little because the inflammation is deeper. Oral antihistamines are more effective. Systemic steroids should only be used with medical supervision.
Can emotional stress alone cause hives?
Stress is rarely the only cause, but it is a powerful trigger. It sensitizes mast cells and increases histamine release. Relaxation techniques can reduce outbreak frequency in susceptible people.
Do children get hives for the same reasons as adults?
Yes, but viral infections and new foods are more common triggers in children. Most cases are mild and self-limited, but recurrent episodes should be evaluated.
Final Thoughts
Hives are not just a random skin irritation. They are a signal from your body that something is out of balance.
By identifying triggers, acting quickly with antihistamines, and tracking patterns, you can regain control of your skin — and your peace of mind — without unpleasant surprises in the mirror each morning.
Your skin speaks. Learning to listen can spare you a lot of itching.